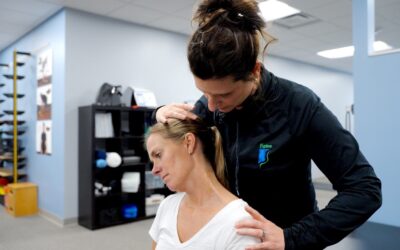
Parent's Guide: Understanding and addressing back-to-school back pain Back pain is just something that happens as you get older, right? It’s such a common reference to aging that we joke about with each trip around the sun. So, it’s rare to worry about your child...
Pain Management FAQs
Your guide to chronic pain—frequently asked questions from patients in pain Chronic pain is one of the most common reasons people seek medical care, because it can impact every aspect of your life, not just your physical state. Even though chronic pain is widespread,...
Exercises for Golfers
Hit the links without hurting this year—what are the best exercises to support golfer’s backs? In a recent blog post, we went over the most frequent injuries golfer’s experience, and what commonly causes them. In today’s article, we’d like to discuss the best...
Pain Management Resources
You don’t have to hurt—find the resources you need to successfully manage chronic pain It’s normal—and unavoidable—to experience pain in your life. From everyday bumps and bruises to acute injury events, you will hurt here and there, and those incidents can usually be...
Shopping Cart Syndrome
What does the grocery store have to do with back pain? What shopping cart syndrome means for your spine. Imagine you are grocery shopping. Ignore all the other shoppers; don’t worry about the employees stocking the shelves. I want you to imagine pushing the cart—what...
Golf & Back Pain
Hit the links without hurting—why does golf cause back pain? The familiar motions of a golf swing in the spring sunshine can be a powerful mood lifter—there’s a reason golf is so popular here in the Twin Cities. But with that positivity can come an unwelcome side...
Joint Mobilization Therapy
What are Joint Mobilization Techniques? Joint Mobilization techniques are hands-on treatment methods for pain management and mobility therapy. The primary goal of a joint mobilization is to improve the range of motion of the joint and surrounding tissues. The...
Cognitive Behavioral Training
Pain in the Brain: How does pain work? It is common to think that pain is a result of tissue injury. You scrape your knee and it hurts. As the tissues heal, the pain goes away. But did you know, that how intense the pain is, how long it lasts, if it starts to spread,...
iSpine Clinics Builds Resiliency to Pain
Pain is complicated. Many factors affect how a person feels and functions. iSpine Rehab Clinics provides patients an opportunity to explore their contributors to pain, learn new skills, and build new habits so they may be more resilient to pain and function better....
Lower Back Pain Treatment (part 3)
Relief is on the horizon – Different options for treatment of lower back pain We’ve reached the final portion of our low back pain blog series! In previous blogs, we discussed the potential causes of lower back pain, as well as the symptoms, both obvious and...